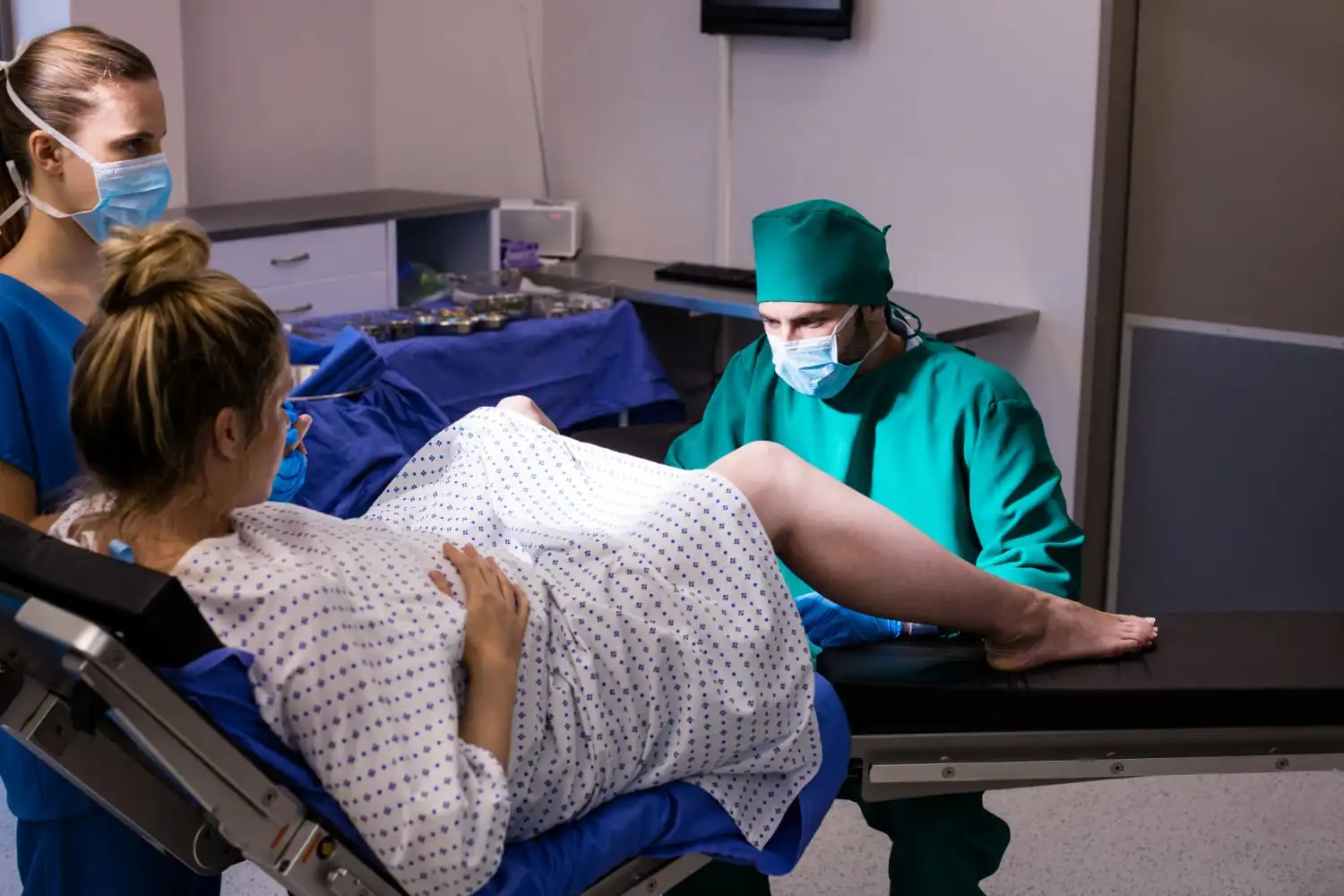
What Are the Types of Delivery in Pregnancy?
1. Vaginal Delivery
A. What is a Vaginal Delivery?
B. Types of Normal Vaginal Delivery
A vaginal delivery can occur in two ways: Spontaneously or through Induction.
i. Spontaneous Vaginal Delivery: This is a natural delivery process that occurs without the need for labor-inducing drugs. Ideally, it takes place around the 40th week of pregnancy when labor begins naturally.
ii. Induced Vaginal Delivery: In this method, labor is initiated through the use of medications or other techniques to stimulate contractions and prepare the cervix for delivery. Pregnancy care providers may recommend induction when a pregnant individual has a medical condition or has exceeded their due date. Typically, labor is induced using a synthetic form of oxytocin called Pitocin.
C. Benefits of Vaginal Delivery
The benefits of a vaginal delivery are:
- Quicker recovery.
- Safest for both the mother and the unborn child.
- Lower infection rates.
- Infants have a stronger immune system and are less likely to experience respiratory issues.
- Most of the time, lactation and breastfeeding are simpler.
D. Risks
Although vaginal birth is a common procedure there are certain risks involved:
- Vaginal tearing while you are giving birth
- Tearing between your vagina and anus
- Pain during sexual intercourse
2. Assisted Vaginal Delivery
A. What is Assisted Vaginal Delivery?
During an assisted vaginal delivery, your obstetrician employs specialized instruments like forceps or a vacuum device to facilitate the safe delivery of your baby through the birth canal.
B. Types of Assisted Vaginal Delivery
The circumstances that develop throughout your labour will have an impact on the course of action that your obstetrician recommends. Methods of assisted delivery that might be used include:
i. Forceps Delivery: This technique gently grasps your baby’s head with surgical tools like tongs to help them pass through the birth canal. Some benefits of choosing a forceps delivery include:
- Reduced risk of injury and infection for the mother.
- Shorter hospital stay for the mother.
- Faster and less painful recovery for the mother.
- Lower blood loss during the procedure.
- Absence of complications related to surgery.
- Lower risk of breathing difficulties for the baby.
C. Risks of a Forceps-Assisted Vaginal Birth
Compared to a natural vaginal birth, a forceps-assisted delivery may bring some concerns and potential risks to both the mother and the baby:
Risks for the Baby:
- Increased likelihood of short-term marking or bruising on the baby’s cheeks.
- Though rare, there is a possibility of more complex injuries.
Risks for the Mother:
- Higher chances of experiencing vaginal tearing or a small cut (episiotomy) that may require stitches.
- Possibility of injury to the muscle around the rectum (bowel).
- Temporary issues with bladder or bowel control.
- Short-term pain during intercourse.
Expectant parents need to be aware of these potential risks and discuss them with their healthcare provider to make informed decisions about the birthing process.
ii. Vacuum Extraction Delivery: In this method, a little suction cup is placed on the head of your baby, and a pump is used to gently traction your baby while you continue to push.
Vacuum extraction and forceps delivery share similar advantages and drawbacks, and the selection between these methods often hinges on the expertise of your obstetrician.
3. Cesarean Section
In a C-section birth, the obstetrician delivers the baby through surgical incisions in the abdomen and uterus. This procedure may be planned if there are medical reasons or might be unplanned due to certain issues during labor. In the United States, approximately 1.2 million C-section deliveries occur each year.
Advantages of a caesarean section include a reduced risk of urinary and fecal incontinence, avoidance of labor pain, and a lower chance of complications associated with vaginal delivery.
On the other hand, there are some risks involved:
For the baby:
- Short-term breathing difficulties
- Short-term breastfeeding difficulties
For the mother:
- Longer recovery period
- Increased bleeding
- Potential injury to bladder or bowels
- Chances of getting a wound infection
- Elevated pain levels
4. VBAC (Vaginal Birth After Cesarean)
A. What is VBAC?
B. Benefits of VBAC
Opting for a successful VBAC can offer several advantages, including:
- Quicker recovery: A shorter hospital stay allows you and your baby to return home earlier. Additionally, you may experience less pain and regain normal activities faster compared to a C-section.
- Reduced risk of complications: VBAC may decrease the chances of infection, bleeding, and other surgery-related complications.
- Lower risk of breathing issues for the baby.
Moreover, choosing VBAC for your next pregnancy might lead to fewer risks and potentially a faster labor process.
C. Risks of VBAC
Experiencing a Cesarean section leaves a lasting mark on the uterine wall, rendering the scarred area comparatively weaker than the surrounding tissue.
Opting for a Vaginal Birth After a Cesarean (VBAC) comes with a potential risk: the scar from the prior C-section may reopen during labor and delivery, resulting in a condition known as “uterine rupture.” While the likelihood of this occurrence is relatively low, approximately 0.5-1%, it remains a critical concern as it could lead to severe, life-threatening complications for both the mother and the baby.
5. Water Birth
A water birth involves the mother experiencing childbirth stages in a portable tub similar to a hot tub. The baby can be born underwater, or the mother can change positions. Women choose water births for relaxation and reduced pain. Birthing tubs are used in homes and birthing centers, and some hospitals also offer them.
Advantages of water birth include potential pain reduction and a more relaxed experience. The water allows for natural and less painful positions, and partners can join to support the delivery.
Critics suggest possible infection risks, but with clean water, the risk is no higher than non-water births. Setting up and warming the tub can be challenging outside established birth centers. Complications may require hospital transfer if the home birth plan deviates from the norm.
Pre-Delivery Tips
When it comes to having a healthy delivery, expecting moms need to take some important steps. Taking good care of yourself during pregnancy is vital for both you and your baby. Regular prenatal care, a balanced diet, and staying active through exercise prepare your body for the demands of labor. Going for prenatal check-ups helps identify and manage any potential complications, making delivery safer.
Using Personal Health Record (PHR) apps and health lockers can make things easier. These digital tools give you quick access to your medical information, like past pregnancies, allergies, medications, and test results. By keeping your records up-to-date, your healthcare professionals can better understand your health, provide you with better care, and make informed decisions throughout your pregnancy and delivery journey. Being actively involved in tracking your medical history empowers you to contribute to a healthier and safer pregnancy experience.
Remember, keeping a record of your medical history during pregnancy is crucial. It helps your healthcare providers make informed decisions and offer personalized care, ensuring a positive and successful childbirth experience.
Get the Health-e app now and take charge of your pregnancy journey! Easily track your medical history and get personalized care for a healthier and safer delivery.
Final Thoughts
There are several types of delivery options available to pregnant women. Each method has its own benefits and risks, and it’s important for expectant mothers to discuss their options with their healthcare providers. Whether it’s a vaginal birth, a cesarean section, or an assisted delivery, the ultimate goal is to ensure the safety and well-being of both mother and baby.
By understanding the different types of delivery and being aware of the available resources and support systems, women can make informed decisions that align with their preferences and medical needs. Remember, every pregnancy is unique, so it’s essential to have open and honest conversations with your healthcare team throughout your journey.